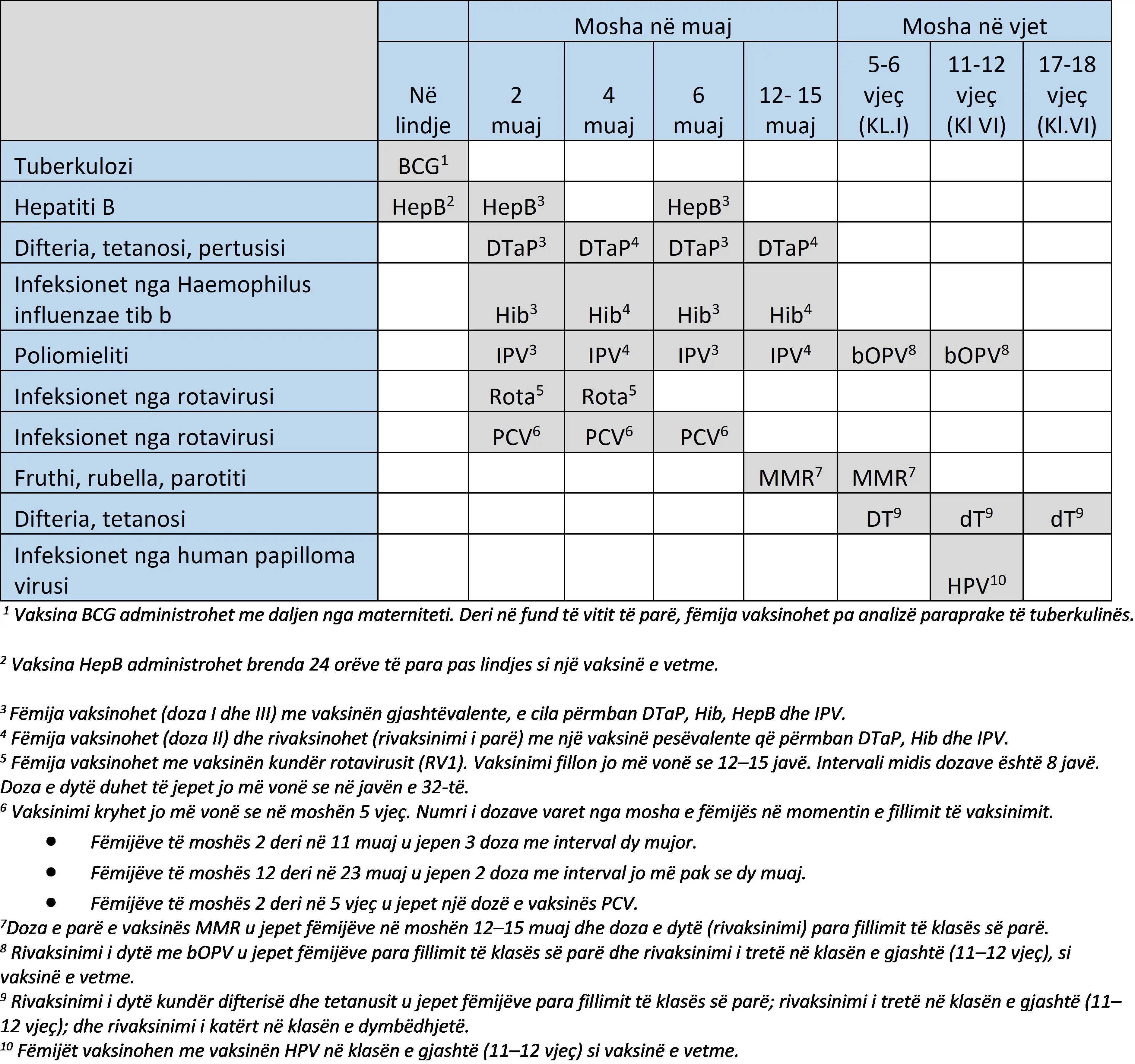
Imunizimi është mënyra më e sigurt për të mbrojtur shëndetin tuaj dhe të të dashurve tuaj. Vaksinat na ndihmojnë të parandalojmë sëmundje serioze dhe të mbrojmë jetën. Në çdo hap, vaksinat janë të rëndësishme për të siguruar një të ardhme të shëndetshme për të gjithë komunitetin tonë.

-
-
- 02 Dec 2026
Find the vaccination point in the respective municipality
Our team of dedicated medical experts
Healthcare blogs provide valuable information for maintaining good health.

Çfarë është HPV dhe si mund të transmetohet?
HPV është virus (virusi i papillomës humane) i cili infekton lëkurën ose mukozën. Në disa raste infeksioni shkakton shfaqjen e papillomave (rritje që duken si lytha).
HPV përhapet nga personi i cili e ka virusin përmes kontaktit të drejtpërdrejtë me lëkurën e infektuar, mukozën ose lëngjet trupore. Në raste të rralla, HPV mund të bartet nga nëna e infektuar tek foshnja e porsalindur gjatë lindjes.
Sa shpesh është e përhapur HPV dhe kush është në rrezik më të madh për infeksion?
HPV është njëri ndër virusët më të përhapur. Sipas statistikave, ku deri në 80% e popullates dmth 8 në 10 meshkuj dhe femra do të infektohen me një ose me më shumë lloje të HPV-së gjatë jetës së tyre. Të rinjtë janë në rrezik më të madh ndaj infektimit.
A mund të ndodhin komplikime serioze si pasojë e infeksionit me HPV?
Infeksioni me ndonjë lloj të HPV-së me rrezikshmëri të lartë mund të shkaktoj ndryshime jonormale në qelizat që rrethojnë qafën e mitrës. Këto quhen ndryshime (ose lezione) parakanceroze. Nëse nuk shërohen ose nuk largohen, mund të zhvillohen në kancer. Duhen disa vite që këto ndryshime të zhvillohen në kancer të qafës së mitrës.
Faktori i rrezikut më i rëndësishëm është infeksioni me ndonjë lloj të HPV-së me rrezikshmëri të lartë. Faktorët tjerë të rrezikut përfshijnë moshën e re të shtatzënisë së parë, tri ose më shumë shtatzëni të plota, pirja e duhanit, sistemi imunitar i dobësuar ose infeksioni me HIV.
Kanceri i qafës së mitrës është njëri nga kanceret më të shpeshta te femrat me rreth 66 000 raste dhe 30 000 vdekje të regjistruara në vit në Rajonin Evropian të OBSh-së. Në vitin 2020 në mbarë botën janë raportuar rreth 600 000 raste të kancerit të qafës së mitrës dhe 341 000 vdekje për shkak të kancerit të qafës së mitrës.
Ndryshe nga shumica e kancereve tjera, kanceri i qafës së mitrës ka më shumë gjasa të zhvillohet tek femrat e moshes 20-45 vjeçare krahasuar me gratë më të moshuara.
Shumica e rasteve ndodhin në vendet ku nuk ka program të komletuar të skriningut për kancer të qafës së mitrës (të cilat zbulojnë dhe trajtojnë rritjet parakanceroze dhe kancerin e hershëm para se të përparoj).
Cilat janë llojet e ndryshme të HPV dhe cilat janë ato që shkaktojnë më shumë shqetësime?
Ekzistojnë mbi 200 lloje të HPV-së. Secili lloj ka një numër të caktuar sipas radhës kur është zbuluar.
Shumica e infeksioneve me HPV nuk kanë simptoma të dukshme dhe mund të kalojnë pa u vënë re. Megjithatë, disa lloje shkaktojnë ndjesi të dukshme si papilomat në zona të ndryshme të trupit.
Disa lloje të HPV-së, të njohura si lloje me rrezikshmëri të lartë (16 dhe 18) mund të shkaktojnë kancer të qafës së mitrës dhe kancere tjera. Llojet e HPV-së me rrezikshmëri të ulët mund të shkaktojnë lytha të zakonshëm, veruka (lytha në shputën e këmbës), lytha në rajonin gjenital ose në raste të rralla rritje të ngjashme me lytha në rrugët e frymëmarrjes (duke shkaktuar çrregullim të zërit të quajtur Papillomatoza Respiratore Rekurente ose PRR).
Si ndihmon vaksina kundër HPV në mbrojtjen nga lloje të ndryshme të virusit?
Vaksina HPV mund të parandalojë më shumë se 90% të kancereve të ndërlidhura me HPV-në. Vaksinimi me HPV është ndër masat më efektive në parandalimin e kancerit të qafës së mitrës më vonë gjatë jetës nëse administrohet tek mosha nga 9 deri në 14 vjeçare. Vaksina HPV rekomandohet të administrohet te kjo grupmoshe me 1 dozë. Vaksina HPV është efektive dhe e sigurt. Në momentin e vaksinimit, personat mund të përjetonë dhimbje në vendin e injektimit por zakonisht kalon menjëherë pas dhënies së vaksinës. Vaksina HPV u jepet si prioritet vajzave, por gjithashtu në shumë vende është në dispozicion edhe për djemtë. Vakina HPV është aprovuar në vitin 2006 ku nga atëherë shumë shtete Evroiane kanë filluar së implementuari në programet e tyre të vaksinimit. Nga marsi 2023, 45 (nga 53) vende në Rajonin Evropian të OBSh-së ofrojnë vaksinim HPV për vajzat, dhe në 20 nga ato vende ofrohet edhe për djemtë. Vaksina kundër HPV-së ndihmon në parandalimin e infeksioneve nga llojet më të rrezikshme të virusit. Ajo është efektive në reduktimin e incidencës së kancerit të qafës së mitrës dhe sëmundjeve të tjera të lidhura me HPV. Vaksinimi me HPV në kombinim me kontrollet e rregullta ofrojnë mënyrën më efektive për femra për t'u mbrojtur nga kanceri i qafës së mitrës.
Verifikimi i infeksionit me HPV
Testimi për HPV është i rëndësishëm për të identifikuar infeksionet e rrezikshme dhe për të parashikuar kancerin e qafës së mitrës në faza të hershme. Ai zakonisht realizohet si pjesë e ekzaminimeve gjinekologjike në kuadër të kontrollave rutinore si pjesë e skriningut, ku merren mostra qelizore nga qafa e mitrës.
PAP testi gjegjësisht strisho vaginale (SMEAR TEST) përdoret për të zbuluar rritjet abnormale të qelizave (lezione parakanceroze ose kanceroze). Inspektimi vizual dhe testi HPV përdoren për të zbuluar llojet me rrezikshmëri të lartë të HPV-së të cilat mund të shkaktojnë kancer.
Këto teste përdoren në programet e skriningut për kancer të qafës së mitrës për të zbuluar rritjet parakanceroze dhe kancerin e hershëm, kështu që ato mund të trajtohen para se të përparoj kanceri.
Fatkeqësisht, programet e skriningut nuk mund të zbulojnë ose parandalojnë të gjitha rastet e kancerit të qafës së mitrës. Edhe në vendet me program efektiv të skriningut për kancer të qafës së mitrës kanë numër të konsiderueshëm të vdekjeve nga kanceri i qafës së mitrës.
A mund të parandalohet infeksioni i HPV dhe kanceri i qafës së mitrës?
Rreziku nga kanceri i qafës së mitrës mund të zvogëlohet shumë përmes vaksinimit me kohë me HPV dhe skriningut të qafës së mitrës.
Vaksinimi me HPV ul ndjeshëm rrezikun nga infeksioni sepse vaksinat mbrojnë kundër llojeve më të shpeshta të HPV-së, të cilat shkaktojnë deri në 9 nga 10 raste të kancerit të qafës së mitrës dhe 9 nga 10 raste të lythave gjenitale. Vaksinimi me HPV nuk do të mbrojë kundër të gjitha llojeve të HPV-së, kështu që skriningu për kancer të qafës së mitrës është ende i rëndësishëm edhe nëse një grua është vaksinuar.
Skriningu i qafës së mitrës mund të zbulojë lezionet parakanceroze dhe kancerin e qafës së mitrës në fazë të hershme kur trajtimi ende mund të jetë i suksesshëm. Vendet me programe kombëtare të skriningut kanë zvogëluar incidencën e kancerit invaziv (të avancuar) të qafës së mitrës. Fatkeqësisht, skriningu nuk mund të parandalojë ose zbulojë të gjitha rastet e kancerit të qafës së mitrës. Edhe vendet me program efektiv të skriningut të kancerit të qafës së mitrës kanë numër të konsiderueshëm të vdekjeve nga kanceri i qafës së mitrës.
Kjo është arsyeja se pse vaksinimi në kombinim me kontrolla të rregullta ofron mënyrën më efektive për femra për tu mbrojtur nga kanceri i qafës së mitrës.
Skriningu duhet të bëhet tek të gjitha moshat e sidomos tek femrat mbi 30 vjeç. Infeksioni HPV mund të zgjasë dhe me kalimin e kohës të shkakton ndryshime në qafën e mitrës të cilat mund të zhvillohen më pastaj në kancer të qafës së mitrës. Zakonisht duhen 15-20 vite që kanceri i qafës së mitrës të zhvillohet tek gratë me sistem imunitar normal dhe deri në 5 vite tek gratë të cilat janë të sëmura dhe me sistem të dobësuar imunitar. Zbulimi dhe trajtimi i hershëm i lezioneve prekanceroze parandalon zhvillimin e kancerit të qafës së mitrës. Kanceri i qafës së mitrës i cili zbulohet në fazë të hershme mund të trajtohet në mënyrë efektive. Prandaj, OBSh rekomandon skriningun për gratë e vaksinuara si dhe ato të pavaksinuara, duke filluar nga mosha 30 vjeçare dhe përsëri çdo 5-10 vite, ose çdo tre vite kur përdoret inspektimi vizual ose citologjik si test parësor i skriningut deri në moshën 49 vjeçare. Për individët të cilët janë HIV pozitiv, skriningu duhet të fillojë në moshën 25 vjeçare dhe të përsëritet çdo 3-5 vite. Nëse gjatë testimit gjenden qeliza prekanceroze të qafës së mitrës, trajtimi përfshin një procedurë minimalisht invazive për të shkatërruar qelizat anormale në qafën e mitrës. Kanceri i qafës së mitrës trajtohet me kirurgji, terapi me rrezatim dhe kimioterapi. Nëse nuk ofrohet trajtimi me kohë, kanceri i qafës së mitrës mund të jetë fatal.
Në Kosovë vaksinimi me HPV ka filluar në shkur të vitit 2024. Vaksina HPV ka hyrë në kalendarin e rregull të vaksinimit si vaksine e obliguar. Vaksina HPV administrohet te fëmijët e moshës 11-12 vjeçare gjegjësisht te nxënësit e klasës gjashtë. Deri tani në Kosovë janë administruar mbi 10,000 doza të vaksins HPV.
I. SËMUNDJA SHKAKTUAR NGA PNEUMOKOKU
1. Çka është pneumokoku?
Pneumokoku, i quajtur edhe Streptococcus pneumoniae, është bakter që zakonisht gjendet në hundën dhe fytin e personave të shëndosh pa shkaktuar sëmundje. Mund të përhapet në pjesë të ndryshme të trupit për të shkaktuar disa sëmundje, njëra prej tyre është pneumonia. Streptococcus pneumoniae është shkaktari kryesor i pneumonisë bakteriale.
2. Çfarë sëmundje shkakton pneumokoku?
a) Infeksionet e rënda të njohura si sëmundja pneumokokut invazive (SPI) ndodhin kur pneumokoku hyn në qarkullimin e gjakut (bakteremia) dhe më pas përmes qarkullimit të gjakut mund të infektojë vendet tjera në trup. SPI rezulton në sëmundshmëri dhe vdekshmëri të konsiderueshme. SPI përfshinë:
b) Sëmundjet më pak të rënda, por më të zakonshme ndodhin kur pneumokoku përhapet lokalisht nga nazofaringu në veshë, sinus dhe bronket aty pranë dhe përfshijnë:
3. Sa janë të shpeshta sëmundjet shkaktuara nga pneumokoku?
Llojet më të zakonshme të infeksioneve së pneumokokut përfshijnë infeksionet e veshit të mesëm, infeksionet e sinusit, pneumoninë, baktereminë dhe meningjitin.
Sëmundjet e shkaktuara nga Streptococcus pneumoniae përbëjnë problem të madh global të shëndetit publik. Në vitin 2000, u vlerësuan të ndodhin rreth 14.5 milionë episode të sëmundjes së rëndë pneumokokale (varg 11.1-18.0 milionë), duke rezultuar në rreth 826 000 vdekje (sfera: 582 000-926 000) te fëmijët e moshës 1-59 muajshe, nga të cilat 10006:3000. 0) ishin me HIV-pozitiv dhe 735 000 (varg: 519 000-825 000) në fëmijët HIV-negativ. Nga vdekjet e fëmijëve HIV-negativ, mbi 61% kanë ndodhur në dhjetë vende afrikane dhe aziatike.
4. Kush është në rrezik të shtuar nga pneumokoku?
5. Si përhapet sëmundja e pneumokokut?
Përhapet nga personi në person përmes spërklave të frymëmarrjes (p.sh., për shkak të kollitjes ose teshtitjes). Hunda dhe fyti i deri në 70% të personave të shëndetshëm përmbajnë pneumokok në çdo kohë të caktuar.
6. A mund të trajtohet sëmundja e pneumokokut?
7. Pse i vaksinojmë fëmijët kundër sëmundjes së pneumokokut?
Rreziku nga sëmundja e rëndë të pneumokokut është më i lartë në vitin e parë të jetës, por gjithashtu mbetet i lartë gjatë 24 muajve të parë të jetës. Vaksinimi kundër sëmundjes së pneumokokut është mënyra më kosto efektive për parandalimin e sëmundjes. Vaksinimi mund të parandalojë vdekshmërinë dhe sëmundshmërinë e konsiderueshme në popullatat e pashërbyera të vendeve më të varfra.
Çfarë sëmundje janë fruthi dhe rubella?
Fruthi është sëmundje shumë serioze ngjitëse e cila shkaktohet nga virusi i fruthit. Fruthi mund të komplikohet me pneumoni, verbim, encefalit (infeksion të trurit), diarre të rëndë me dehidrim si dhe infeksion të veshit. Fruthi përhapet përmes spërklave nga hunda, goja ose fyti i personave të infektuar.
Fruthi është njëra prej shkaqeve kryesore të vdekjes tek fëmijët në botë.
Rubella është sëmundje relativisht e lehtë por nëse nëna infektohet gjatë shtatzënisë atëherë mund të shkaktojë deformitet tek fryti gjatë jetës intrauterine ose të shkaktoj abort.
Pse fruthi dhe rubella janë në axhendën e OBSh-së dhe në atë të shëndetit publik?
Pas një periudhe me numër shumë të ulët të rasteve me fruth në Rajonin Evropian të OBSh-së gjatë vitit 2021, nga fillimi i vitit 2022 rastet kanë filluar të rriten pasi që sfidat e vazhdueshme në programin e vaksinimit gjatë pandemisë COVID-19 kanë lënë shumë persona të pavaksinuar mes të cilëve një numër të madh të fëmijëve tek të cilët sëmundja mund të jetë fatale.
Pas shpërthimeve të mëdha të fruthit përgjatë vitit 2018 dhe 2019 ku janë raportuar përafësisht 200 000 raste, ku numri i rasteve të raportuara të fruthit në Rajonin Evropian të OBSh-së në vitin 2020 ka rënë në 12 000. Gjatë vitit 2021 u raportuan vetëm 159 raste të fruthit në 22 vende; megjithatë, ky numër u rrit në vitin 2022 në 904 raste të raportuara deri më sot.
Në Kosovë nuk është regjistruar asnjë rast i fruthit nga viti 2000 deri në vitin 2017. Gjatë viteve 2017-2018 janë regjistruar 749 raste të konfirmuara dhe dy raste të vdekjes nga fruthi. Këto raste dhe vdekje do të mund të ishin parandaluar nëse do të ishin të vaksinuar.
Fruthi nuk është më i zakonshëm. A nevojitet ende vaksinimi?
Numri i rasteve të fruthit kanë rënë në mënyrë drastike gjatë viteve të fundit falë futjes së dy dozave të vaksinës në kalendarin rutinore të imunizimit në të gjithë Rajonin e Evropës. Megjithatë, ende vazhdojnë të paraqiten epidemi të fruthit në vende ku mbulueshmëria me vaksinim është me e ulët. Mbulueshmëria mbi 95% me vaksinim kundër fruthit nevojitet për të mbrojtur popullatën nga fruthi ku përfshihen edhe ata që nuk mund të vaksinohen për shkak të gjendjes së tyre shëndetësore.
A ka ndonjë dëshmi që vaksinimi shkakton autizëm?
Jo! Vaksinimi mbron të gjitha moshat nga kjo sëmundje. Vaksina e fruthit është në përdorim për më shumë se 50 vjet. Është e sigurt, efektive dhe nuk kushton shtrenjtë. Vaksinat kundër fruthit, shytave dhe rubellës (MMR) janë të sigurta dhe shumë efektive sa që me mbulueshmëri të lartë me imunizim mund të eliminojmë këto sëmundje nga i gjithë Rajoni Evropian.
Duke ju falenderuar vaksinave prindërit e fëmijëve të cilët janë vaksinuar plotësisht nuk duhet të shqetësohen nga sëmundjet e rënda si difteria, tetanusi, poliomieliti, fruthi dhe rubella. Duhet të bëjmë çdo përpjekje të ofrojmë informata të bazuara në prova mbi përfitimet e vaksinimit të cilat duhet ti paraqesim në mënyrë që ti kuptoj publiku. Këto informata duhet të vijnë nga burime të besueshme dhe të shpërndahen përmes gjitha kanaleve mediatike.
Duke e vaksinuar fëmijën tuaj ose veten ju do të mbroni fëmijët, familjen, komunitetin dhe vendin tuaj nga fruthi dhe rubella si dhe do të kontribuoni në eliminimin global të fruthit në mbarë botën.
Por, kam lexuar se ka prova që vaksina MMR shkakton autizëm?
Autizmi paraqet shqetësim të madh për shëndetin publik prandaj nevojitet të kuptojmë më mirë shkaqet e tij. Shumë studime të ndërmarra në mënyrë strikte ku janë përfshirë qindra mijëra fëmijë me qëllim që të hulumtohet nëse ka lidhje të mundshme mes vaksinës MMR dhe autizmit ose çrregullimeve autike, përfundimisht nuk ka gjetë lidhje të tillë. Në vitin 2002, Komiteti Global Këshillimor për Sigurinë e Vaksinave bëri një rishikim të gjerë të njëmbëdhjetë studimeve epidemiologjike (duke përfshirë këtu studimin e bazuar në popullatë në Danimarkë me mbi 500,000 fëmijë të cilët përfaqësojnë pothuajse 100% të fëmijëve të lindur gjatë asaj periudhe) dhe arriti në përfundim se nuk ekziston asnjë provë për ndonjë lidhje mes vaksinës së MMR dhe autizmit ose çrregullimeve autike. Ky studim mund të gjendet në http://www.nejm.org/doi/full/10.1056/NEJMoa021134
Po me sëmundjet tjera?
Garantimi i sigurisë dhe cilësisë së vaksinave është njëra nga prioritetet kryesore të OBSh-së. Para se të mund të licencohet çdo vaksinë vlerësohet dhe testohet në mënyrë gjithëpërfshirëse për t'u siguruar se është e sigurt dhe efikase. Çdo grup i vaksinave kontrollohet veçmas para se të përdoret dhe monitorimi i tyre për efekte anësore është një proces i vazhdueshëm që zhvillohet si në nivelin lokal por edhe në atë global. Reaksionet e zakonshme, si skuqja dhe dhimbja në vendin e injektimit janë të vogla dhe të përkohshme. Efektet serioze shëndetësore pas vaksinimit janë të rralla por tërësisht të hulumtuara. Nëse EPPV dyshohet se ka ndonjë ndërlidhje me vaksinimin atëherë ndërmerren hapa të menjëhershëm për të adresuar shkakun. Në shumicën dërrmuese të rasteve këto rezultojnë të jenë të rastësishme gjatë vaksinimit (që ndodh në të njëjtën kohë por nuk ndërlidhen me vaksinën).
Edhe pse ka studime të shumta hulumtuese që vërtetojnë se vaksinimi nuk shkakton sëmundje, shumë persona besojnë se po. Pse ndodh kjo dhe si mund ta parandalojmë këtë?
Vaksinimi është metoda më efikase e shëndetit publik që kemi në dispozicion për promovimin e shëndetit dhe uljen e barrës së sëmundjeve infektive. Duke ju falenderuar vaksinimit, lija (variolla), e cila dikur vriste 35% të infektuarve ose shkaktonte verbim si dhe pasoja të tjera është eradikuar globalisht. Polio, e cila është sëmundje që shkakton paralizë është ende endemike vetëm në tri vende. Fruthi dhe rubella janë eliminuar nga i gjithë rajoni i OBSh-së në Amerikë dhe rrallë hasen në Evropë në vendet me mbulueshmëri të lartë me vaksinim. Rreziqet serioze shëndetësore që ato paraqesin për fëmijët dhe të rriturit e pavaksinuar pothuajse janë harruar.
Trajtimi i hezitimit për vaksinim është thelbësor jo vetëm për vaksinim në afat të shkurtër, por edhe për sigurimin e qëndrueshmërisë së popullatës ndaj thashethemeve dhe dezinformatave në të ardhmen.
A është e rrezikshme t'u jepen fëmijëve vaksina të kombinuara si MMR (kundër fruthit, shytave dhe rubellës)?
Provat shkencore tregojnë se administrimi i disa vaksinave në të njëjtën kohë nuk ka asnjë efekt negativ në sistemin imunitar të fëmijës. Në fakt, vetëm përmes frymëmarrjes dhe ngrënies fëmijët ekspozohen çdo ditë ndaj disa qindra substancave të huaja që shkaktojnë përgjigje imune. Vaksinat e kombinuara rekomandohen meqenëse ato mundësojnë: kursimin e kohës dhe mjeteve (parave); vizita më të rralla në institucionet e kujdesit shëndetësorë; zvogëlon shqetësimin për fëmijën me më pak shpime; rrisin probabilitetin që fëmija të vaksinohet plotësisht sipas kalendarit të rregullt.
Çka nevojitet për të eliminuar fruthin dhe rubellën?
Për të eliminuar një sëmundje kërkohet imunitet i lartë i popullatës ndaj asaj sëmundje. Mbulueshmëria me vaksinim në pupullatë duhet të jetë mbi 95% me dy doza të vaksinës kundër fruthit-shytave-rubellës (MMR). Aty ku shkalla e vaksinimit është më e ulët se 95%, numri i personave të pambrojtur rritet me kalimin e kohës, duke e lënë komunitetin gjithnjë e më shumë në rrezik nga shpërthimet në shkallë të gjerë.
Eliminimi gjithashtu kërkon sistem të mbikëqyrjes me cilësi të lartë, që të zbulohen rastet e dyshuara sa më herët dhe të verifikohen me teste laboratorike. Në këtë mënyrë rastet e dyshuara mund të konfirmohen me qëllim që masat e kontrollit mund të nisin shumë shpejt. Testet specifike laboratorike gjithashtu lejojnë identifikimin dhe karakteristikat e transmetimit të sëmundjes brenda dhe jashtë vendeve.
Cilat janë sfidat kryesore për eliminimin e fruthit dhe rubellës?
Njëra nga sfidat kryesore është arritja dhe ruajtja e mbulueshmërisë së lartë të popullatës me vaksinim me së paku 95% me dy doza të vaksinës.
Derisa shumica e prindërve i vaksinojnë fëmijët e tyre, disa të tjerë vendosin që të shtyjnë vaksinimin ose edhe madje të mos i vaksinojnë ata fare. Mos vaksinimi i fëmijëve të tyre i vendos ata në rrezikshmëri të lartë për t'u prekur nga fruthi në moshën kur ata janë veçanërisht të ndjeshëm ndaj komplikimeve serioze të sëmundjes.
Nëse femrat në moshën e lindjes mbeten të pavaksinuara dhe infektohen nga rubella gjatë shtatzënisë, ato mund të abortojnë ose foshnjat e tyre mund të zhvillojnë deformime të rënda kongjenitale si humbje të dëgjimit, verbëri dhe defekte të zemrës.
Sfidë tjetër është që mbikëqyrja e këtyre sëmundjeve të bëhet mjaft mire me qëllim për të siguruar se rastet e dyshimta të raportohen dhe mostrat e mbledhura të testohen në laboratore kompetente. Pasi që këto sëmundje janë bërë më pak të zakonshme, punëtorët shëndetësorë janë më pak të njohur me karakteristikat e tyre klinike.
Zbulimi i vonshëm i rasteve e rrit rrezikun e përhapjes dhe e vonon fillimin e masave të shëndetit publik për të kontrolluar shpërthimin (siç është hetimi i kontakteve për vaksinim të mundshëm).
A duhet të shqetësohen personat që udhëtojnë në Evropë ose jetojnë në rajon për shpërthime të mundshme të fruthit? Çka mund të bëjnë ata për të shmangur virusin?
Duke qenë se fruthi mbetet endemik në shumicën e pjesëve të botës, ai mund të përhapet kudo, duke përfshirë edhe vendet ku është eliminuar. Çdo person i rrezikuar duhet të marrë dy doza të vaksinës së fruthit në mënyrë që të jetë i imunizuar plotësisht.
Në Rajonin Evropian, dy të tretat nga 53 vendet, territoret dhe zonat e kanë ndërprerë transmetimin endemik të fruthit. Megjithatë, mënyra e sotme e udhëtimit e vënë në rrezik çdo person apo vend, territor apo zonë për mundësnë e infektimit me virusin e fruthit. Shpërthimet do të vazhdojnë në Evropë, si kudo tjetër, derisa çdo komunitet të arrijë nivelin e imunizimit të nevojshëm për të mbrojtur plotësisht popullsinë e tyre.
Autoritetet shëndetësore duhet të maksimizojnë përpjekjet e tyre për të arritur dhe/ose mbajtur të paktën 95% të mbulueshmërisë me 2 doza të vaksinës MMR për të parandaluar qarkullimin në rast të importit.
Çka duhet të bëjmë ne të gjithë në mënyrë individuale dhe kolektive?
Për të arritur eliminimin rajonal të fruthit dhe rubellës ne duhet të tregojmë përkushtim ndaj eliminimit duke ndërmarrë më shumë veprime për:
• të arritur ≥ 95% mbulueshmëri të imunizimit me dy doza të fruthit dhe të paktën një dozë të vaksinës kundër rubellës;
• të mbyllur boshllëqet e imunitetit në të gjitha grupmoshat;
• zbulimin e hershëm të rasteve dhe shpërthimeve të dyshuara përmes mbikëqyrjes;
• t'u siguruar profesionistëve shëndetësorë dhe publikut informata të mirëfilltë mbi përfitimet dhe rreziqet që ndërlidhen me vaksinimin kundër fruthit dhe rubellës;
• të sigurojë që programet e imunizimit të kenë qasje të qëndrueshme në financim të planifikuar dhe furnizim me cilësi të lartë.
Ku mund të gjej më shumë informata?
Mund ti gjeni në linqet më poshtë:
Webfaqja e OBSh-së për fruthin: https://www.who.int/health-topics/measles#
Webfaqja e OBSh-së për rubellën: https://www.who.int/news-room/fact-sheets/detail/rubella
Video e OBSh-së rreth 5 gjërave që duhet të dini për fruthin: https://www.who.int/health-topics/measles#
Pyetje të shpeshta rreth vaksinës së Gripit
A është e sigurt vaksina e gripit?
Vaksina e gripit është e sigurt dhe rekomandohet për të gjithë personat mbi moshën 6 muajshe. Personat që nuk duhet të marrin vaksinën e gripit janë ata që kanë pasur reaksion të rëndë alergjik ndaj vaksinës së gripit ose ndonjë vaksine tjetër në të kaluarën, si dhe ata që kanë pasur sindromën Guillain-Barré.
Nëse keni pyetje për gjendjen tuaj specifike shëndetësore, telefononi mjekun tuaj për të pyetur nëse është e sigurt për ju të merrni vaksinën e gripit.
A mund të sëmurem me grip nga vaksina e gripit?
Jo, vaksina e gripit nuk mund të shkaktojë sëmundjen e gripit. Vaksinat e gripit që jepen me gjilpërë (injeksion) prodhohen në dy mënyra:
a) me viruse gripi të mbytura (të inaktivizuara) dhe për këtë arsye nuk janë infektuese, ose
b) me proteina nga virusi i gripit në vend të virusit të plotë (si në rastin e vaksinës rekombinante kundër gripit).
Vaksina me spraj nazal përmban viruse të gjalla të dobësuara (atenuara), por gjithashtu nuk shkakton grip. Këto viruse janë të përshtatura për të vepruar në temperatura të ulëta, që do të thotë se ato shkaktojnë infeksion vetëm në temperaturat më të ftohta si brenda hundës. Ato nuk mund të infektojnë mushkëritë apo zona të tjera me temperaturë më të lartë.
Cilat efekte anësore mund të shfaqen pas vaksinimit?
Edhe pse vaksina nuk shkakton grip, mund të ketë disa efekte anësore të lidhura me vaksinën me injeksion ose me spraj nazal. Këto efekte janë zakonisht të lehta dhe afatshkurtra, sidomos krahasuar me simptomat e një rasti të rëndë gripi.
Vaksina me injeksion:
• Dhimbje, skuqje dhe/ose ënjtje në vendin e injektimit
• Dhimbje koke (e lehtë)
• Temperaturë
• Dhimbje muskujsh
• Të përziera
• Lodhje
Vaksina me spraj nazal – tek fëmijët:
• Rrjedhje hundësh
• Fishkëllimë në frymëmarrje
• Dhimbje koke
• Të vjella
• Dhimbje muskujsh
• Temperaturë (e lehtë)
Tek të rriturit:
• Rrjedhje hundësh
• Dhimbje koke
• Dhimbje fyti
• Kollë
Nëse këto probleme ndodhin, akonisht fillojnë menjëherë pas vaksinimit, janë të lehta dhe kalimtare. Vaksina me injeksion, si edhe injeksionet e tjera, ndonjëherë mund të shkaktojë sinkopë. Njoftoni personelin shëndetësor nëse ndjeni marramendje ose keni ndryshime në shikim apo zhurmë në veshë. Si me çdo ilaç, ekziston një mundësi shumë e rrallë për reaksion të rëndë alergjik, dëmtime serioze ose vdekje.
Si funksionojnë vaksinat e gripit?
Vaksinat e gripit bëjnë që trupi të prodhojë antitrupa rreth dy javë pas vaksinimit. Këta antitrupa ofrojnë mbrojtje kundër infeksionit nga viruset që përfshihen në vaksinë.
Vaksina sezonale e gripit mbron kundër viruseve të gripit që sipas studimeve pritet të jenë më të zakonshmet gjatë sezonit të ardhshëm. Shumica e vaksinave në Shtetet e Bashkuara janë “katërvalente” (quadrivalente) dhe mbrojnë kundër katër viruseve të ndryshme: një virus Influenza A (H1N1), një virus Influenza A (H3N2) dhe dy viruse Influenza B. Ka gjithashtu vaksina “trevalente” që mbrojnë kundër tre viruseve: Influenza A (H1N1), Influenza A (H3N2) dhe një virus Influenza B. Dy nga vaksinat trevalente janë përfituar posaçërisht për personat 65 vjeç e lart për të krijuar një përgjigje më të fortë imunitare.
Kur duhet të vaksinohem?
Duhet të vaksinoheni para se viruset e gripit të fillojnë të përhapen në komuniteti, pasi duhen rreth dy javë që trupi të zhvillojë mbrojtje. Planifikoni të vaksinoheni herët në vjeshtë, përpara fillimit të sezonit të gripit. CDC rekomandon që njerëzit të vaksinohen deri në fund të tetorit. Megjithatë, vaksinimi shumë herët (p.sh. në korrik ose gusht) mund të shoqërohet me mbrojtje të reduktuar më vonë gjatë sezonit, sidomos tek të moshuarit. Vaksinimi duhet të vazhdojë gjatë gjithë sezonit, madje edhe në janar ose më vonë. Fëmijët që kanë nevojë për dy doza duhet ta fillojnë më herët, sepse dozat duhet të jepen me të paktën katër javë diferencë.
Pse duhet të vaksinohemi çdo vit?
Vaksina nevojitet çdo sezon për dy arsye:
Së pari, mbrojtja imunitare bie me kalimin e kohës, kështu që kërkohet vaksinë vjetore për mbrojtje optimale.
Së dyti, viruset e gripit ndryshojnë vazhdimisht, prandaj vaksinat përditësohen nga një sezon në tjetrin për të mbrojtur kundër viruseve në qarkullim. Për mbrojtje më të mirë, të gjithë personat 6 muajsh e lart duhet të vaksinohen çdo vit.
A funksionon vaksina menjëherë pas aplikimit?
Jo. Duhet rreth dy javë që trupi të prodhojë antitrupa dhe të krijojë mbrojtje kundër infeksionit nga virusi i gripit.
A duhet të vaksinohem nëse jam shtatzënë ose ushqej me gji?
Vite studimesh dhe vëzhgimesh tregojnë se vaksina me injeksion është e sigurt në çdo tremujor të shtatzënisë dhe gjatë ushqyerjes me gji. Foshnjat nuk mund të vaksinohen deri në moshën 6 muajsh. Antitrupat kalojnë tek fetusi përmes placentës dhe tek foshnja përmes qumështit të gjirit, duke e mbrojtur atë.
Gratë shtatzëna nuk duhet të marrin vaksinën me spraj nazal. Personat me alergji të rrezikshme për jetën ndaj vezës nuk duhet të marrin vaksinën e gripit, pavarësisht nëse janë shtatzënë apo jo.
A mund të sëmurem nga gripi edhe pse jam vaksinuar këtë vit?
Po, është e mundur të sëmureni edhe nëse jeni vaksinuar. Kjo mund të ndodhë sepse:
• Mund të jeni ekspozuar ndaj virusit pak para vaksinimit ose gjatë periudhës kur trupi po zhvillon mbrojtje.
• Mund të jeni ekspozuar ndaj një virusi që nuk përfshihet në vaksinë.
• Disa persona mund të infektohen edhe me një virus që vaksina synon të mbrojë, për shkak të faktorëve si mosha dhe gjendja shëndetësore.
Megjithatë, vaksinimi mbetet mënyra më e mirë për t’u mbrojtur nga gripi.
Çfarë mbrojtjeje ofron vaksina nëse sëmurem gjithsesi?
Studimet tregojnë se vaksina mund të zvogëlojë ashpërsinë e sëmundjes, rrezikun e shtrimit në terapi intensive dhe kohëzgjatjen e qëndrimit në spital.
Cilat janë përfitimet e vaksinës kundër gripit?
• Parandalon sëmundjen nga gripi
• Zvogëlon rrezikun e shtrimit në spital tek fëmijët, të rriturit dhe të moshuarit
• Është mjet i rëndësishëm për personat me sëmundje kronike
• Zvogëlon rrezikun e komplikimeve kardiake
• Zvogëlon përkeqësimin e sëmundjeve kronike të mushkërive
• Zvogëlon shtrimet në spital tek personat me diabet
• Mbron gratë gjatë dhe pas shtatzënisë
• Mund të shpëtojë jetën e fëmijëve
• Zvogëlon ashpërsinë e sëmundjes edhe nëse infektoheni
A do të ketë grip dhe COVID-19 në vjeshtë dhe dimër?
Është e mundur që të dy viruset të përhapen njëkohësisht. Prandaj vaksinimi kundër gripit është shumë i rëndësishëm.
A mund të kem grip dhe COVID-19 në të njëjtën kohë?
Po. Simptomat janë të ngjashme dhe testimi diagnostik ndihmon për të përcaktuar saktë sëmundjen.
ëaksina e gripit a e parandalon COVID-19?
Jo, por ndihmon në uljen e rrezikut të sëmundjes së rëndë duke parandaluar gripin e rëndë.
A e rrit vaksina e gripit rrezikun për COVID-19?
Nuk ka prova që vaksina e gripit rrit rrezikun për t’u sëmurë me koronavirus. Studime të mëvonshme kanë treguar se vaksinimi nuk rrit rrezikun për infeksione të tjera respiratore.
Ku është vendi më i sigurt për t’u vaksinuar nëse jam me rrezik të lartë?
Mund të vaksinoheni në mënyrë të sigurt në qendrat e mjekësisë familjare. Kur shkoni për t’u vaksinuar, ndiqni masat e zakonshme parandaluese.